It’s been said before that the American healthcare system is one giant workaround. In some areas, innovation is able to fix broken incentives and create a more sensible structure. In others, innovation means creating new workarounds; ones that improve the patient experience but fail to resolve the underlying systemic issues.
Digital pharmacies are an example of the latter. In the past few years, companies like Ro, Hims, and Nurx have taken off by allowing patients to order medications online and receive them in the mail. Instead of going to your doctor for a prescription, these pharmacies connect you with licensed providers virtually, who review your medical history and then prescribe your medication. Between the three of them, patients are able to get everything from erectile dysfunction pills to antidepressants to HPV screening tests, without leaving their home. This seems like a no-brainer from a patient perspective, so what makes them another workaround?
Digital pharmacies don’t provide proper medical supervision
When an FDA approves a new drug, the default option is to restrict it to prescription use only, mitigating the risk of the drug being used by patients it was not intended for. In special cases, where the safety and efficacy of a drug is clear even without medical supervision, it can be approved for over-the-counter (OTC) use as well.
The first common thread between most of the products offered by digital pharmacies is that they are approved for prescription use only and not for OTC use. This makes sense, as the value proposition for digital pharmacies is significantly stronger for prescription only medications. With OTC drugs (think Tylenol, Advil), patients can go to a local CVS and pick them up, no questions asked, so the value add for digital pharmacies would just be saving patients a 30-minute commute. With prescription drugs, however, digital pharmacies are saving patients the hassle of scheduling and waiting for a doctor visit, and in some cases (think ED, birth control), the stigma of having to talk to someone in-person.
The issue with digital pharmacies is that the virtual doctor interactions that they offer before prescribing medications are not an adequate replacement for in-person visits. The process patients go through, where providers review their medical information and prescribe the medications they are looking for, feels more like a formality than an actual evaluation. In fact, because their biggest pitch to consumers is convenience, digital pharmacies are actually incentivized to make the process as quick and easy as possible. Given that the medications being prescribed require “medical supervision” by law, this raises the serious question of whether digital pharmacies increase safety risks to patients.
The risk to patients is low, but growing
Thus far, these companies have limited themselves to medications that are well characterized from a safety standpoint and indications that are largely self-diagnosable. On the former, given the tenuous regulatory framework, the greatest threat to their business model is a headline about a serious patient complication that invites regulatory oversight. Focusing on medications that are well understood mitigates this risk. Additionally, as D2C companies, digital pharmacies rely heavily on direct patient demand, so they need to work off medications that patients are already familiar with and trust.
On the latter, the lack of in-person visits means that digital pharmacy providers need to be able to identify a medical need without an in-depth evaluation. This has led to a focus on indications that can largely be self-diagnosed — think erectile dysfunction, anxiety + depression, hair loss, birth control, etc. These are also indications where the potential risk to patients in the event of a misdiagnosis is minimal.
However, as digital pharmacies continue to grow, this concern of patient safety will intensify, as companies expand their offerings to cover higher risk medications and conditions. It’s important to note that these companies aren’t technically doing anything wrong at the moment, and in fact, are just taking advantage of regulatory ambiguity and ambivalence. But their success does raise regulatory questions that should be answered sooner rather than later.
FDA should provide clarity, one way or another
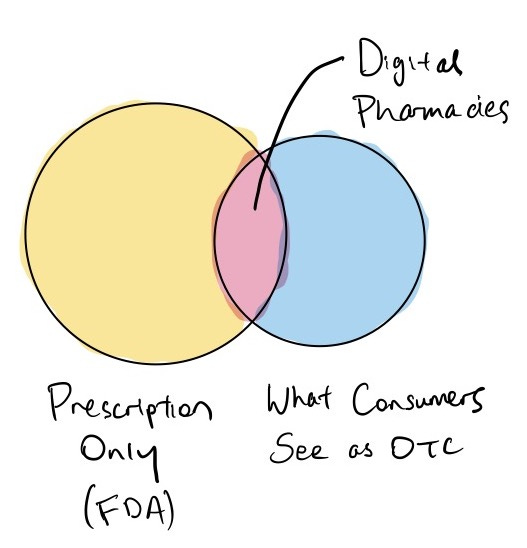
The fundamental insight that digital pharmacies have realized is that there is a disconnect between what the FDA regulates as prescription only vs OTC and what consumers want as OTC. The overlap — prescription only medications that consumers wish were OTC — is the market for these companies.
The regulatory dilemma is this: If these medications are truly safe and effective without a prescription, FDA should loosen oversight and make them OTC. If these medications are not safe and effective without a prescription, FDA should tighten oversight and make it clear that a couple of text messages with a doctor in the same state does not constitute medical supervision. The reason I say digital pharmacies are a workaround is that, in either of these worlds, they would not exist.
One way or another, FDA should provide more clarity on what medical supervision means for medications in this grey area. The agency’s silence has spawned the success of a whole segment of digital health companies. But in this case, they are taking advantage of a broken system, rather than improving it.




Interesting subject and analysis. Personally, I think even in either market they will still survive due to making process simpler. Would love to hear your take.
Getting an appointment for simple prescription is time consuming unless healthcare providers use telehealth or phone to make it easier. Hims actually will send prescription to nearby pharmacy and Nurx focuses on specific segment. These companies are driving market segmentation by focusing in one area coupled with best interface and customer service.